PCOS and PCOD are terms almost every woman has heard, but very few truly understand. While they sound similar, these two conditions are quite different. Knowing how they differ can help women take charge of their hormonal health, recognise symptoms early, and make confident lifestyle decisions.

How PCOS Develops: A Simple Breakdown of the Mechanism
PCOS doesn’t begin from just one cause, it develops through a mix of genetic factors, metabolic changes, hormonal imbalances, and lifestyle triggers. Here’s a clear explanation of how the condition actually develops inside the body.
1. Genetic & Environmental Triggers
PCOS often starts with internal and external triggers such as:
- Genetic or epigenetic changes
- Changes in how receptors bind to hormones
- Obesity and chronic inflammation
- Exposure to environmental toxins
- Diet, stress, and mood factors
These triggers disrupt normal hormone and metabolic balance.
2. Metabolic Abnormalities
Before hormonal changes appear, metabolic issues begin in the body:
- Reduced glucose uptake in fat cells
- Reduced fat breakdown, causing fat accumulation
- Poor insulin signaling in skeletal muscles
- Reduced glycogen synthesis in the liver
- Changes in IGF-1 levels
All these together lead to insulin resistance, a key driver of PCOS.
3. Insulin Resistance
Because cells don’t respond properly to insulin, the body produces more of it.
This results in hyperinsulinemia, which:
- Stimulates excess androgen (male hormone) production
- Worsens fat storage
- Increases inflammation
Insulin resistance is one of the earliest and most important mechanisms in PCOS.
4. Androgen Overload
High insulin levels cause the ovaries and adrenal glands to produce more androgens.
This leads to:
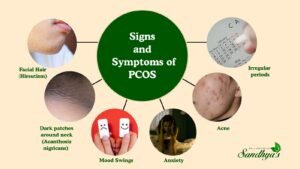
- Acne
- Facial/body hair growth
- Hair thinning
- Irregular ovulation
Androgen overload disrupts the entire reproductive cycle.
5. Brain–Ovary Hormonal Imbalance
PCOS also affects communication between the brain and ovaries:
- The brain releases more GnRH
- The pituitary responds with higher LH
- Adrenal glands release more ACTH
- Ovaries produce more androgens instead of developing mature eggs
This imbalance between LH and FSH prevents normal ovulation.
6. Reproductive Impact
Due to hormone and metabolic disturbances:
- Eggs do not mature properly
- Ovulation becomes irregular or absent
- Multiple immature follicles appear on the ovaries
This leads to irregular periods and fertility challenges.
7. Long-Term Complications
If unmanaged, PCOS may increase the risk of:
- Type 2 diabetes
- High blood pressure
- Heart disease
- Endometrial cancer (in later stages)
This is why early lifestyle modifications are essential
Anthropometric indicators:
Increase in Weight, Waist circumference, Hip circumference, Body mass index(BMI) are evident.
How they diagnose PCOD
Globally accepted diagnostic criteria is Rotterdam criteria(2003) – Must have any 2 out of these 3 criteria:
- Irregular periods/oligo anovulation: >35 days or fewer than 8 cycles per year
- Hyperandrogenism (Excessive androgens)
- Polycystic ovaries on ultrasound – ≥ 12 follicles (2-9 mm in diameter) or increase in ovarian volume
Dietary management:
- Balanced meal proportion
- Seed cycling for balancing the hormones:
-
- 1st day – 15th day of cycle : Flaxseeds- 1 tsp + Pumpkin seeds – 1 tsp
- 16th day – 30th day of cycle: Sesame seeds – 1 tsp + Sunflower seeds – 1 tsp
-
- Anti- inflammatory diet :
-
- Refraining from wheat and wheat products, milk and milk product
- Including Anti-inflammatory foods such as turmeric, black pepper, ginger, garlic, olive oil, nuts and oilseeds, omega-3 foods(walnuts, flaxseeds, fish), green leafy vegetables, fermented foods
-
- Correcting deficiencies such as Vitamin D, Vitamin B12, Iron levels
- Chrono-nutrition strategies
- Eating as per circadian rhythm
- Fixed eating window
- Dinner should be finished 2 hr before bed time
- Cutting down extra sugars
- Stress management
- Adequate sleep (7 to 8 hours a day)
References:
- Lonardo, M. S., Cacciapuoti, N., Guida, B., Di Lorenzo, M., Chiurazzi, M., Damiano, S., & Menale, C. (2024). Hypothalamic-ovarian axis and adiposity relationship in polycystic ovary syndrome: physiopathology and therapeutic options for the management of metabolic and inflammatory aspects. Current Obesity Reports, 13(1), 51-70.
- Hakami, A. A., Hamzi, W. A., Alshammari, H. O., Alshammari, T. O., Aldfeery, F. Z. S., Alanazi, I. S. H., … & Albathali, A. B. S. (2024). Polycystic ovary syndrome (PCOS): Pathophysiology, diagnosis, biomarkers, and nursing interventions.
- Su, P., Chen, C., & Sun, Y. (2025). Physiopathology of polycystic ovary syndrome in endocrinology, metabolism and inflammation. Journal of ovarian research, 18(1), 34.
- Christ, J. P., & Cedars, M. I. (2023). Current Guidelines for Diagnosing PCOS. Diagnostics (Basel, Switzerland), 13(6), 1113. https://doi.org/10.3390/diagnostics13061113














